Also, download this story from the electronic issue here
Technology advances in the medical sector are equated to giving better quality results for treatments and diagnostics. In developing and low to middle-income economies, where spending on medical services is limited and inadequate infrastructure and facilities are concerns, access to advanced medical technologies is almost prohibitive. Thus, this has resulted in innovative and alternative systems, says Angelica Buan in this report.

What is being done with old/used plastics?
There is an enormous unmet need for the design and development of medical devices and technologies for use in the developing world. Fortunately, recent years have seen an explosion of interest and funding for addressing global healthcare inequalities. New technologies are making it possible to develop low-cost diagnostic and therapeutic devices with the potential to make a huge impact.
On the other side, used toys like Lego bricks as moulds for lab-onchips or an old bike pump to run a nebuliser have been repurposed by the Massachusetts Institute of Technology (MIT)’s Innovations in International Health initiative, under the purview of Programme Director, Jose Gomez- Marquez.
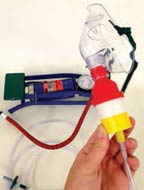
The Honduras-native inventor works with his team at the Massachusetts-based Little Devices Lab, reverseengineering expensive medical devices and rebuilding them using cheap components like used toys. He says that toys and medical devices share commonalities such as being small and precisely manufactured, and highly regulated for safety.
MakerNurse, an initiative launched in September 2013, is also spearheaded by Gomez-Marquez, and is supported by the Robert Wood Johnson Foundation.
The project focuses on innovativeness of nurses when faced with healthcare and medical care delivery challenges. It encourages sharing of practical solutions and technologies that have been developed by nurses to improve a patient’s health.
For instance, to develop further the construction of makeshift intravenous (IV) site protectors using cut-up plastic cups and tape, a safer version of such innovation has been developed. It features a plastic U-shaped domed cup, known as the IV House, which is awaiting a patent application. Improving further for geriatric patients with fragile skin, the invention uses a fabric wrap around the skin instead of tape.
Improvising for practicality
Africa, a country that is also challenged by the high cost of healthcare and limited access to advanced diagnostics, can benefit from frugal innovations.
For instance, Nigerian surgeon, Dr Oluombo Awojobi, has created a blood centrifuge with used bike parts for his farm clinic. The proxy device is pedalled by hand to spin the blood sample.
Awojobi’s 52-bed clinic in Eruwa, a rural area about 60 km from Ibadan in south-western Nigeria, also features other cheap inventions, like a woodmetal operating table covered with formica for a smooth surface, and that can be raised and lowered by a vehicle-use hydraulic jack. A rear wheel of a bicycle, which revolves at 5,400 rpm with a force 3,000 times the force of gravity, is turned into a haematocrit centrifuge. It is used to determine the level of oxygencarrying red cells in patients’ blood.
While the above examples given are commendable, it is always advisable to have the experience and advice of a registered healthcare expert!
US firms cater to lower income groups
Meanwhile, one company that has probably put frugal innovation in the mainstream is US conglomerate General Electric (GE). It started in 2007 making medical devices in India, including ultrasound and electrocardiogram (ECG) machines, and is shipping the lower costing equipment to emerging markets in Africa, Eastern Europe, Latin America and Asia. The company says that the equipment, manufactured at its Bangalore facility, is 40% cheaper.
Meanwhile, the MAC400, GE's first portable ECG, also designed in India, uses less plastic and a smaller LCD screen, thus saving on materials, and costs US$800 against the high-end versions in the US$2,000-US$10,000 range.

California-based D-Rev, a not-for-profit product development company, says it designs medical devices for people living under US$4 a day. D-Rev has innovated the ReMotion Knee, a prosthetic knee that mobilises above-knee amputees, and is worn by more than 4,700 amputees in India and parts of Africa, Asia, and Latin America. The firm, which has an R&D funded by grants from foundations and private sectors, has been cited a Technology Pioneer 2014 in the Health Category by the World Economic Forum San Francisco.
Traditionally, microfluidic devices have been fabricated like microchips using photolithography. A desired pattern of micrometer-sized channels and ports is created on top of a silicon substrate, which can then be replicated many times by moulding or embossing. However, the process requires specialised cleanroom equipment and can take several days to complete.
If valves are needed in the system, they traditionally have been made from silicones, which are not the best materials to use with particular laboratory assays or for manufacturing lab-on-a-chip structures.
The National Institute of Standards and Technology or NIST (an agency of the US Department of Commerce) has spent the past few years developing and refining a method for making microfluidic devices using plastic films and doublesided tape that produces a functional apparatus in hours rather than days, and requires only simple tools to create channels and ports.
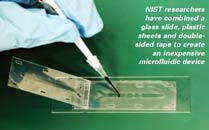
The NIST designs allow for folding the films to make multilayer or 3D structures, can be used to make devices with multiple functions, and cost a fraction of traditional fabrication techniques.
To develop this further, NIST and the University of Maryland have developed an under-US$1 system for a 3D microfluidic device for manufacturing uniformly sized and shaped vesicles or liposomes. It consists of bundled capillary tubes, which the team says requires no special fabrication technology or expertise. The device consists of a 3-mm glass cylinder containing a bundle of seven tiny glass capillary tubes, and a 500-micrometre plastic capillary through the centre tube. Liposomes are simple cell-like spheres made of a double layer of phospholipids, used as artificial drug carriers.
Baby care at a nominal cost
One of D-Rev’s designs is Brilliance, a globallyappropriate phototherapy device to treat newborn jaundice in low-income hospitals, which is half the cost of the lowest-cost incubator and 1/10th of the cost in industrialised markets. It is working with Indiabased neonatal products supplier Phoenix Medical Systems to manufacture and market Brilliance.

Yet another success story comes from a social enterprise known as Embrace Innovations. From what started at Stanford Design School in the US as an idea to create a neonatal hypothermia that cost less than 1% of the price of an incubator, developed to a baby warmer when it was soon realised that costs was just one part of the problem, with shortage of highly skilled caregivers, inadequate power, and maintenance issues adding to the challenge.
Thus, to help millions of vulnerable babies in less developed countries, especially in areas where electricity is unreliable or equipment is scarce, infant warmers were developed.
Embrace Nest is an insulated pouch that is able to keep a low weight baby at a temperature of 37°C while Embrace Care is a completely non-electric baby warmer intended for home use.
Embrace uses the WarmPak, an innovative phasechange material to rapidly stabilise the temperature of an infant suffering from hypothermia, absorbing heat quickly and then releasing it over a long period of time.
Three components are incorporated in the design of the warmer: a sleeping bag, a pouch of phase-change material, and an electric heater to warm the pouch.
In conclusion, it can be seen that various efforts have been exerted into simplifying technologies and lowering costs, while maintaining the quality results that they deliver.
Advocates of low-cost healthcare have helped in bringing frugal innovation concepts, which are usually low-cost medical devices specially designed for low and middle-income economies, to fruition.

Asia improvises with low-cost healthcare; mHealth to emerge
Healthcare spending in Asia Pacific was estimated at about US$1.34 trillion in 2013 and is expected to grow at a CAGR of 10.5% over the next five years to reach US$2.21 trillion in 2018. While the region is going through major regulatory transitions where patient access and reduction of costs are paramount, there are major transformations expected to impact the charter on growth for companies in the future, says Frost & Sullivan in its healthcare report.
With the exception of sophisticated markets of Australia and Japan, other countries are far from introducing regulations that support the use of advanced medical technology products, according to Reenita Das, Senior Vice President of Healthcare and Life Sciences at Frost & Sullivan. She also says that there is a strong pull toward usage of more simplistic frugal products that are “easy to use and require less administration and training time” and adds, “This could mean the only way to introduce high-tech products into these markets would be to develop products that are also low in cost.”
Das gives examples of Indian prosthetic organisations having built prosthetic limbs costing less than US$45 each and used in over 1,000 amputee cases, while Diabeto has built a Bluetoothpowered hardware device for easy monitoring of blood sugar levels for diabetics, costing less than US$50.
At the other end of the scale, Das predicts the high penetration of mobile phone technology across a number of Asia Pacific countries. “By 2020, we’re expected to have approximately 20 billion devices globally. China is projected to have 5.1 billion and India, 1.5 billion. Smartphone penetration in South Korea is at 82.4%, followed by Singapore at 74.2%.”
According to UK-based information provider Visiongain, the mobile healthcare market or mHealth will be valued at US$6.7 billion before the onset of 2015. The mHealth tools also include wearables such as smartwatches, smartphones, and tablets. Visiongain says that connected devices and machine-to-machine technology, as well as mobile network advancements and emergence of lowcost smartphones will accelerate mHealth market growth.
Some examples of technology for mHealth include South Korean electronics firm Samsung’s Galaxy S5 smartphone that features a built-in Heart Rate sensor; Hitachi Europe and Viennabased technology firm MIG’s mobile wi-fi-enabled biometric scanners for patients at the point-of-care.
Indeed, while the overall environment in Asia is extremely complex and dynamic, and, while differences remain between the countries there are major transformations enabling change to create more universal policies and systems across this large region.
(PRA)




















